Behind the scenes of a pediatric mission in Benin with Dr. Tayeb Slaouti.
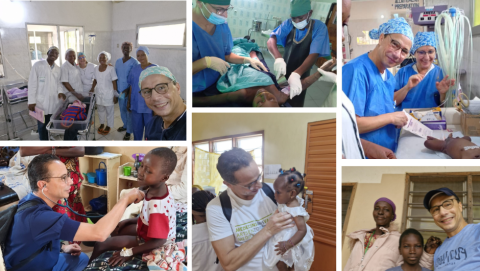
Since 2008, Dr. Tayeb Slaouti, a pediatrician specialized in infectiology and neuropediatrics at the Europe Hospitals, has carried out two weeks of humanitarian missions in Africa every year. With the association Doctors without Vacation, he travels during his holidays to support local pediatric teams. His most recent mission location: the hospital of Bembéréké, in the north of Benin, where premature, dehydrated children or children suffering from malaria struggle to survive in extreme conditions.
The challenge of skin-to-skin care
In African neonatology wards, incubators are rare or old and poorly insulated. “We were faced with premature babies placed on cold metal tables and then in small beds without blankets, without oxygen,” the doctor recounts. “The mothers, for their part, slept on mats outside the neonatology unit, separated from their baby for most of the day.”
Faced with this reality, the objective is to develop a kangaroo unit, meaning to organize care around almost continuous skin-to-skin contact between the newborn and the mother. A simple, humane method with proven effectiveness: better temperature regulation for the newborn, fewer infections, improved nutrition, stronger bonding, and fewer apnea episodes in premature babies.
However, implementing it is long and demanding work.
“The most difficult part is changing mindsets because the ‘Kangaroo’ technique is much more technical than it appears, while still remaining very human. At the beginning, mothers didn’t even have chairs, only stools outside the neonatology ward, then plastic chairs, and finally adapted armchairs. It takes years of diplomacy and training.”
Over the course of the missions, the transformations have become tangible: armchairs installed, teams trained, doctors convinced, and above all… babies who survive with their parents at the heart of their care.
Innovation from the field
Infusions that run too quickly (and are too expensive) cause many deaths every year among malnourished children. Dr. Slaouti therefore proposed a hybrid technique discovered in Rwanda: filling an empty infusion bottle with oral rehydration solution, connecting it to tubing, and then to the nasogastric tube attached to the child. The flow rate is regulated like a classic infusion but requires neither electricity nor a feeding pump, ensuring safe rehydration at a total cost of less than 3 dollars. The benefit: a child rehydrated within four hours, in accordance with the recommendations of the World Health Organization (WHO), without a venous line and without occupying a nurse for hours.
Two months after his departure, the hospital in Bembéréké called him back: the technique had just saved several babies during a gastroenteritis outbreak, and a study will be launched to spread this original oral rehydration technique elsewhere in Benin, or even more widely.
Overflowing corridors
During his mission in Benin, Dr. Slaouti can consult, together with his Beninese counterpart, between 40 and 70 children in one morning. The teams, although deeply dedicated, lack everything: equipment, oxygen, linens, water, and medication.
“We work in pairs with local pediatricians. We share our experiences, we adapt protocols, but we never impose ourselves. They are the ones who provide care all year round. We are only there two weeks per year,” Dr. Slaouti explains.
Stories that leave a mark
Some encounters change an entire mission. Like that of a boy, Raïmi, severely injured in the arm by a machete while working in the fields. The tissues were necrotic, and the limb seemed lost. After 10 days of treatment, the necrosis had healed, but the tissues remained exposed: there was no hope. On the last evening, a German pediatric surgeon arrived asking if there were any pediatric cases. Raïmi was immediately presented to him and a skin graft was attempted over the entire arm. Raïmi returned to visit the team the following year: his arm was saved! He had returned to school and could even bend it.
A similar miracle happened for a 14-year-old girl who had been bitten by a viper. She arrived in shock, with her leg swollen to three times its normal size. The antivenom costs 50 euros per dose — a fortune. Thanks to the responsiveness of the teams and the use of an anti-necrosis antibiotic that had been underused before the mission, she ultimately survived. Her story prompted the hospital management to fund stocks of free snake antivenom for children and pregnant women.
Transmitting, empowering, humanizing
Beyond technical procedures, the mission is above all about transmission.
Training, explaining, supporting, listening, adapting. Building on the strength and knowledge of local teams who work under unimaginable conditions. Supporting without imposing. And leaving while ensuring that the changes continue to save lives.
“It is the smiles of the children, the courage of the parents, and the energy of the caregivers that give us the strength and the desire to return every year,” concludes Dr. Slaouti.

